What Is AED Program Management?Let's assume that you need an AED and prepare to treat a victim of sudden cardiac arrest. However, you soon discover that the device isn’t working. Perhaps the battery is no longer working, or the pads need to be replaced, or the device is past its expiration date. Regardless of what is happening, a non-functional AED is almost worse than no AED at all. To avoid this situation, you might consider AED program management. Facilitating the use of AED program management can assist you with the management of your AEDs through such things as sending you reminders or alerts about upcoming expiration dates while also ensuring you’re meeting legal requirements. What Is An AED? The automated external defibrillator (AED) is a tool used to treat someone who is experiencing cardiac arrest. These life-saving devices analyze the heart rhythm and deliver an electric shock to victims of ventricular fibrillation to restore the heart rhythm to normal. AED's are easy for bystanders to use and you don’t need to be a healthcare provider to operate. AED's are located in various places such as schools, corporate offices, and fitness facilities. In addition, individuals with a high risk of cardiac emergencies might also consider the purchase of one for their home. AEDs dramatically increase a patient’s chance of survival compared to waiting for first responders to arrive, and so it is important that AEDs are accessible in as many places as possible. Why is an AED NEEDED?Over 350,000 cardiac arrests occur outside of the hospital annually. AEDs are an effective way to treat victims of cardiac arrest and can help restore a normal heartbeat in just minutes. These powerful, life-saving devices can improve a patient’s chance of survival considerably compared to CPR alone. What IS AED Program Mangement?Have you purchased an AED for your organization and installed it? Do you think that's all that you need to do? Not exactly. First, you need to set up CPR and First Aid training to ensure that everyone is familiar with the AED. Next, you will need to set up an AED program management schedule which is a service that can allow AED owners to effectively manage their devices. An AED management program typically includes general maintenance, expiration reminders, legal compliance checks, readiness checks, and more. These procedures will help ensure that your AED is fully operational at all times. What are the benefits of aed program management?Establishing an AED program management plan with a reputable AED servicing company like Help-A-Heart CPR is a vital way to ensure that your AED is always functional. There are many benefits to AED management. Here a just a few of the top reasons: 1. Conserve Time. The management and routine inspection of an AED can be time-consuming. Between component replacement, regular inspections, scheduling training, and more, the routine tasks associated with AED maintenance can quickly become overwhelming. Therefore, an AED maintenance program can take over the routine tasks for your organization and/or business allowing you to concentrate on other aspects of your organization. 2. AED Readiness. As we previously discussed, it’s important that AEDs are always operational. The checklists that we will include in your AED program management will help you confirm that everything is up to date and that your AED is operational and safe to use whenever it is needed. 3. Legal Compliance. Maintaining the federal and state requirements for AEDs can be a nuisance and timely. Our AED management program at Help-A-Heart CPR will regularly check the legislature so that you don’t have to and make sure that your AED is compliant. 4. Maintenance Reminders. With AED program management there is not a need to set calendar reminders or rely on your memory. The AED management team will alert you whenever it’s time for maintenance. This is especially convenient if you are responsible for multiple devices across a large facility and need to keep track of various expiration dates. 5. Peace of Mind. Lastly, with the incorporation of AED management at your organization or business, you’ll never have to wonder whether your AED is safe to use. By working with a team of professionals such as Help-A-Heart CPR experts, you can rest easy knowing that everything is taken care of. Contact UsHelp-A-Heart CPR can assist you with AED program management or the purchase of an AED. Our team here at Help-A-Heart CPR has decades of experience with AEDs and we’re happy to help answer any questions you have. We offer comprehensive AED management services to make AED ownership simple.
Do you still have more questions? For more information about our AED program management or any of our other services, please contact us directly. You can contact us through our online form or by phone at 210-380-5344.
Comments
How To Pass The BLS Class!Are you planning to take an AHA or American Red Cross Basic Life Support (BLS) certification course? It’s always a good idea to being preparing for a BLS training class ahead of time. Through a bit of preparation and study, you should be more than prepared to be successful in that upcoming BLS course. What Is The BLS Certification?The American Heart Association (AHA) and the American Red Cross (ARC) oversee the BLS certification curriculum which helps prepare medical professionals to respond to life-threatening emergencies. The BLS certification is recommended and often mandatory for healthcare providers including doctors, nurses, EMTs, dentists, pharmacists, and more. BLS training provides healthcare providers with the skills and knowledge to keep a patient alive until they can arrive at the hospital. So, what do you learn in BLS training? Basic life Support (BLS) training covers topics in emergency life support such as CPR for patients of all ages, treatment for choking victims, proper AED use, and much more. It’s an essential training course for any individual who is looking to pursue a career in the healthcare industry. How To Prepare For the BLS Class?If you haven't taken a BLS class before, there are a few steps you can take to optimize your learning experience. 1. Locate The Appropriate Training When deciding to get your BLS certification, there are several options available. For example, Help-A-Heart CPR CPR provides two methods of BLS training: traditional, instructor-led courses and hybrid online BLS courses with a brief in-person skills check. Some students enjoy the immersion of an in-person course, while others with a busier schedule often prefer the flexibility of a hybrid class. Both paths offer exceptional, high-quality instruction, it’s just a matter of what learning style you prefer and what fits into your schedule. Typically, experienced providers tend to favor the hybrid class, while those new to healthcare enjoy the instructor led option so they can ask the instructor loads of questions! 2. Make A List Of Questions As you begin to study topics relating to BLS, take notes of any questions that you have. Bring a list of your questions with you to the BLS training course so that you can ask the instructor. Having your list ready to go allows you to focus on the course itself and not worry about remembering all your questions. 3. Begin Reviewing Basic BLS Information While any BLS training course will cover all of the necessary information needed to pass the exam and receive the certification, it is always advised to prepare. Prior to participating in the BLS class, take some time to review all things BLS and find out what concepts and topics will be covered in a BLS course. 4. Participate In A Practice Exam. An additional helpful idea is to take a practice exam prior to your BLS class. While you might not be able to pass the practice exam with flying colors until you’ve actually completed the training, it can still be helpful to get a sense for what topics will be covered, what kinds of questions will be on the exam, and how exam questions might be formatted. There are lots of practice exams available for free online. Get Your BLS Certification With Help-A-Heart CPRAre you ready to sign up for an AHA BLS certification course? Register today with Help-A-Heart CPR. We pride ourselves on being a learning center, not a testing center. You will love our laid back, low stress environment so you can get the most out of your training and be 100% ready to save a life! With expert-led instruction, cutting-edge equipment, and engaging lessons, our team can help you get BLS certified.
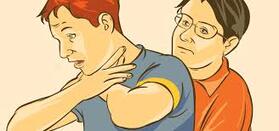
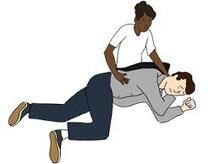
Our team is here to assist you any way we can, so don’t hesitate to contact us with any questions. You can message us online via our contact form or call us at (210) 380-5344. When Do You Use An Abdominal Thrust?When someone is choking, it is important to immediately help them dislodge the object in the airway. The longer that the object stays lodged in the airway, the more precarious the situation becomes. A lifesaving measure used in these situations is the abdominal thrust which can be used to dislodge the object restore normal breathing. So what exactly is an abdominal thrust? Abdominal thrusts are a life-saving technique that both bystanders and first responders can use to treat choking victims. An abdominal thrust allows a rescuer to administer a quick but strong thrust to a choking victim’s abdomen to help force the object out of the airway. What is An Abdominal thrust?Abdominal thrusts, also known as the Heimlich maneuver, are a first-aid technique used to treat conscious choking victims in which the rescuer administers thrusts to a patient’s upper abdominal region. This skill is commonly taught during basic life support (BLS) and advanced cardiac life support (ACLS) classes, but it never receives as much attention as chest compressions and rescue breaths do. The abdominal thrust maneuver can be performed in both children and adults via different techniques. The thrusting motion pushes air from the lungs in an upward motions through the throat to dislodge foreign objects and treat upper airway obstructions. Abdominal thrusts are relatively simple to perform and don’t require any equipment or extensive training. Once you learn the proper technique and abdominal thrust hand placement, anyone can perform them. They’re a quick and accessible way to help a choking victim. Although there are no absolute contraindications, the abdominal thrust maneuver is not recommended by the AHA for infants or unconscious patients. Also, pregnant subjects should receive management with sternal compressions, as opposed to abdominal. How To Perform Abdominal thrustsSo how do you perform an abdominal thrust? To give an abdominal thrust, you should follow the steps below:
ABDOMINAL Thrust FAQ'sWhen should you not use the abdominal thrust? The abdominal thrust maneuver should not be performed on unconscious patients (who should receive chest compressions) or infants (who should receive backslaps). Does an abdominal thrust hurt? Abdominal thrusts can be painful, but that doesn’t mean you should hesitate to deliver them if a patient is choking. The most commonly reported complications are rib fractures and gastric or esophageal perforations. Was the Heimlich maneuver replaced with the abdominal thrust? Yes. The Heimlich maneuver was replaced by abdominal thrusts in the 2006 guidelines by the American Red Cross and the American Heart Association. How can a rescuer tell the difference between mild airway obstruction and severe airway obstruction? The rescuer should ask, “Are you choking?” If the victim nods yes, assistance is needed. Choking also often is indicated by the Universal Distress Signal (hands clutching the throat). Learn CPR With Help-A-Heart CPRWould you like to learn more about abdominal thrusts and other topics related to CPR and First Aid? Take a moment to view our training class schedule where you can also register directly for a CPR or First Aid course with Help-A-Heart CPR!
To find out more, contact us today through our online contact form or give us a call at (210) 380-5344. How To Pass The ACLS Provider Exam!Are you a healthcare provider and preparing to take the American Heart Association (AHA) ACLS Provider course? if you are enrolled in the AHA ACLS class, you might also be wondering how difficult the ACLS Provider Exam is? Our goal here at Help-A-Heart CPR is to help our student's be successful and achieve their various milestones. That's why we created this blog post to guide you along the way. What IS acls?The American Heart Association's Advanced Cardiovascular Life Support (AHA ACLS) course has been created for healthcare providers who either directly or indirectly participate in the resuscitation of a patient, whether in or out of hospital. The ACLS course will allow providers to enhance their skills in the treatment of the adult victim of a cardiac arrest or other cardiopulmonary emergencies. ACLS also emphasizes the importance of basic life support to patient survival; the integration of effective basic life support with advanced cardiovascular life support interventions; and the importance of effective team interaction and communication during resuscitation. ACLS Exam Preparation Hints When you take the AHA ACLS certification course, throughout the course, the instructor will review the information that you need to pass the exam. However, we have provided a few tools and tips below to optimize your learning success. A. Review the ECG Rhythms. A review of the ECG rhythms is critical to success in the ACLS course. Often times, students struggle with ECG rhythm recognition during ACLS. So, if you feel that your knowledge of EGG rhythms is a bit lacking; you may to rake a ECG refresher course prior to taking the ACLS course and exam. If you have additional experience in telemetry and ECG, this might help take a bit of pressure off when you’re going through the ACLS class. However, a review of ECG rhythms is often recommended for everyone. ECG rhythms can sometimes be a little overwhelming, so reviewing the basic rhythms and their corresponding pharmacology will just increase your confidence and your ability to be successful on the ACLS Provider exam. B. Study the AHA ACLS Algorithms. One of the most important things to memorize for the exam is the AHA 2020 ACLS algorithms. It is beneficial to memorize all of these algorithms so that you pass the exam with flying colors. The AHA ACLS algorithms are available in the required AHA 2020 ACLS provider manual so purchase the book prior to the class and review extensively. The AHA 2020 ACLS algorithms are as follows: Acute Coronary Syndrome Algorithm Adult BLS Algorithm Adult Bradycardia Algorithm Adult Cardiac Arrest Algorithm Adult Suspected Stroke Algorithm Adult Tachycardia Algorithm Intermediate Post-Cardiac Arrest Care Algorithm Opioid-Associated Life-Threatening Emergency Algorithm Unstable Tachycardia Algorithm C. Memorize Medications and Doses The AHA ACLS exam will also assess your knowledge and understanding of ACLS medications and dosages. In order to memorize these prior to your exam, you might want to try writing out flashcards, creating mnemonic devices, or using online quiz games. The following are the ACLS medications you might need to know: 1. Adenosine 2. Amiodarone 3. Atropine 4. Dopamine 5. Epinephrine 6. Lidocaine 7. Magnesium 8. Nitroglycerine 9. Morphine D. Take The American Heart Association Pre-Course Self Assessment. The AHA ACLS pre-course self-assessment is an assessment tool with 50 questions that can be taken prior to the actual class. This self-assessment will serve as a tool to gauge your own knowledge of BLS, pharmacology, ECG rhythms, airway management, and the related AHA ACLS algorithms. The AHA ACLS pre-course self-assessment can be accessed here. Learn ACLS Online With Help-A-Heart CPRAre you now ready to take the ACLS exam? Getting an AHA ACLS certification has never been easier than with the ACLS online course. We offer a hybrid class in which you can take a self-paced series of online training modules. Then, just head to our training center for a brief skills practice. It’s a great way to fit training into your busy schedule as a healthcare professional and learn from the comfort of home.
If you’d prefer to learn in-person, we also offer traditional classroom courses. We have multiple convenient locations in Texas and a variety of course times to meet your training needs. We’re here to help you get certified, so feel free to reach out. Contact us via our online form or give us a call at (210) 380-5344. Is CPR Needed For Respiratory Arrest?So you've determined that a patient or victim is unconscious but they have a heart rate and they are breathing on their own. How do you know if it is cardiac arrest of respiratory arrest? Respiratory arrest is a life-threatening situation in which immediate intervention is needed. However time is critical so it is essential to understand the type of arrest the patient is experiencing and begin treatment as soon as possible. Let's look at what respiratory arrest is and causes and possible treatment. Additionally, an early assessment and recognition intervention is important. Further, knowledge and participation of CPR/AED/First Aid training will equip you with the answers to these questions. What is Respiratory Arrest?Respiratory arrest occurs when a patient has stopped breathing. During respiratory arrest, the body is no longer getting oxygen to the brain, heart, and other vital organs. Cardiac arrest almost always follows unless respiratory function is rapidly restored. Occasionally, the patient will have already been experiencing respiratory distress that has gone unidentified or untreated, ultimately developing into respiratory arrest. What Causes respiratory Arrest?A patient may experience respiratory arrest when the nerves and muscles cannot support respiration. There are many potential causes of this, including: 1. COVID-19 2. Head, chest or other major injury 3. Drug overdose 4. Sepsis 5. Neuromuscular diseases such as ALS 6. Stroke 7. Pneumonia What Is The Difference Between respiratory arrest and cardiac arrest?Sometimes, respiratory arrest can lead to cardiac arrest, and other times the two can occur at the same time. In both respiratory and cardiac arrest, the patient will be unconscious and will not be breathing. However, the difference between cardiac and respiratory arrest is that in cases of respiratory arrest, the patient will have a detectable pulse as the heart is still functioning and pumping blood throughout the body. Sudden cardiac arrest (SCA) is when a patient is experiencing an electrical disturbance in the heart, which will interrupt the heart’s rhythm and potentially halt heart function, breathing, and consciousness. Blood flow will stop, and so during sudden cardiac arrest, the patient will not have a strong pulse. How Do You Treat A person in Respiratory arrest?The first responder should assess the emergency and begin an intervention once respiratory arrest is identified. Treatment should focu on supporting the patient while the lungs heal. The goal of supportive care is getting enough oxygen into the blood and delivered to your body to prevent damage and removing the injury that caused Acute Respiratory Distress Syndrome (ARDS) to develop. Instead of administering CPR, you’ll want to follow basic life support (BLS) practices. The following are some of the steps that can be taken to help manage respiratory arrest: 1. Open the airway 2. Apply bag-mask ventilation 3. Prepare for an advanced airway 4. Use the head tilt/chin lift maneuver if there is no cervical spine injury 5. Use the jaw thrust maneuver if there is a potential injury to the cervical spine 6. Check that you are providing sufficient oxygenation 7. Avoid over-ventilation 8. Monitor the pulse for any signs of cardiac arrest Get your BLS Certification With Help-A-Heart CPR!Any healthcare professional or laymen rescuer who might encounter a cardiovascular emergency at home or at their place of employment should participate in a BLS Provider certification with Help-A-Heart CPR. The expert team here at Help-A-Heart CPR can help answer any questions you may have––because we’ve been out on the field treating respiratory arrest and more as EMTs, paramedics, and nurses ourselves.
Key CPR Numbers and Ratios!There are a few important numbers to remember when learning CPR. From the rescue breathing rate for infants and children to the CPR compression rate for adults, it’s important to know and understand the correct parameters. CPR RatiosThere are a few key statistics on CPR ratio and CPR rate for adults, children, and infants that we will highlight. These numbers are based on the latest research from the American Heart Association (AHA) as of November 2021. COMPRESSION/VENTILATIOn |
AuthorDr. Tracy A. Jones is the CEO of Help-A-Heart CPR, LLC and an American Heart Association, ASHI, and American Red Cross Master Program Trainer, Instructor, & AHA Faculty Member located in San Antonio, Texas. Archives
February 2024
Categories |
Help-A-Heart CPR, LLC | 1747 Citadell Plaza Suite 101 | San Antonio, Texas 78209 | (210) 380-5344 | info@helpaheartcpr.com
Copyright © Help-A-Heart CPR, LLC 2024
100% Certification Acceptance
We promise your employer, school, or agency will accept the certification card we issue to you. If there is a question of acceptance or validity, simply send us an email at info@helpaheartcpr.com with full details. We will reach out to the individual/entity and provide accreditation information. If still there’s a question, we will provide you with a full refund of your class fee. It’s that simple.
We promise your employer, school, or agency will accept the certification card we issue to you. If there is a question of acceptance or validity, simply send us an email at info@helpaheartcpr.com with full details. We will reach out to the individual/entity and provide accreditation information. If still there’s a question, we will provide you with a full refund of your class fee. It’s that simple.
|
Communities Served
ALABAMA: Birmingham
ARKANSAS: Fayetteville, Hot Springs, Jonesboro, Little Rock NEW MEXICO: Albuquerque TENNESSEE: Knoxville TEXAS: Amarillo, Arlington, Austin, Bandera, Bastrop, Boerne, Brownsville, Comfort, Converse, Corpus Christi, Dallas/Ft. Worth, Del Rio, Dripping Springs, El Paso, Floresville, Fredericksburg, Georgetown, Harlingen, Houston, Junction, Katy, Kerrville, Kingsville, Kingwood, Laredo, Lubbock, Lufkin, McAllen, Midland, New Braunfels, Odessa, Pleasanton, Round Rock, San Angelo, San Marcos, Schertz, Seguin, Taylor, Temple, Texarkana, Tyler, Universal City, Victoria, Waco, The Woodlands |
Why Choose Help-A-Heart CPR?
1. Flexible Scheduling
2. On and Off Location Training Available 3. Casual, Fun Atmosphere 4. Best Price Guarantee 5. All Instructors are AHA and/or ARC certified 6. 5 Star Google Reviews 7. Blended Learning (Online & Skills Check) Available 8. Meets OSHA & College CPR Requirements 9. Get Certified Within 3-4 Hours 10.Certification Is Good For Two Years 11. Official AHA/ARC/ASHI Training Site 12. High Quality Safety Training! |